Supraclavicular Block
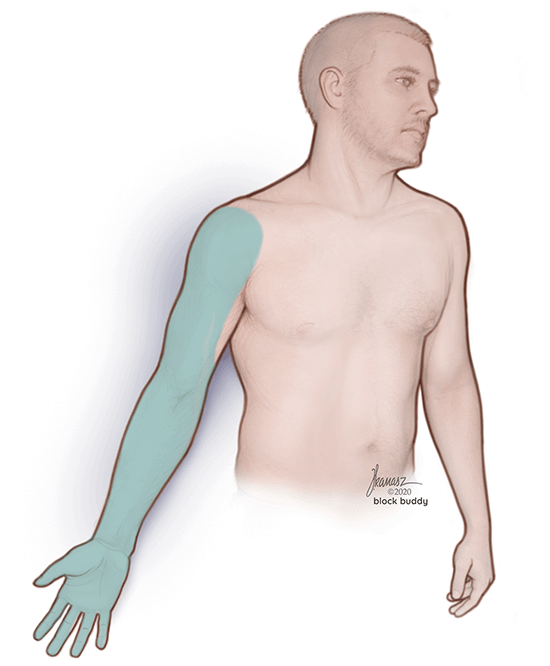
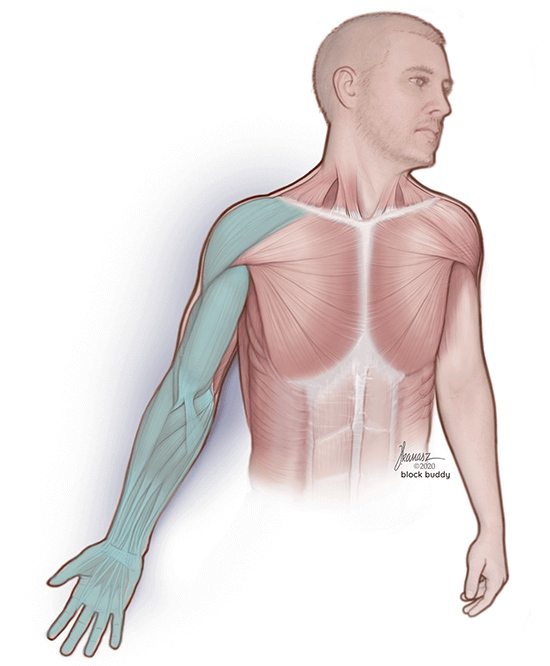
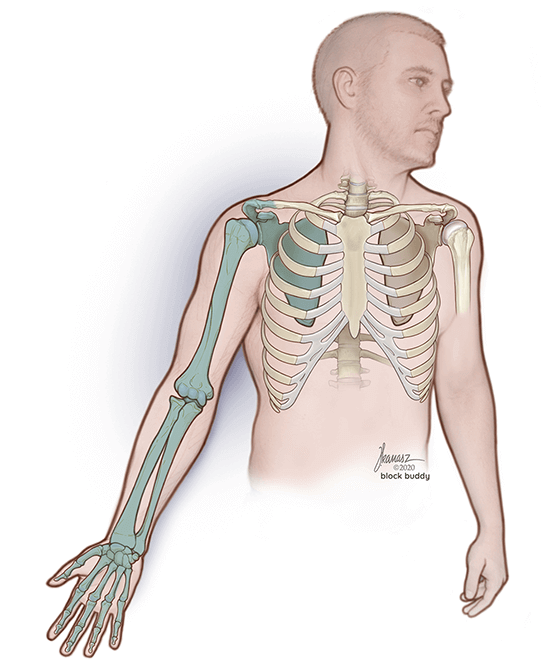
The supraclavicular block, also known as the spinal of the arm, is a regional anesthesia technique that targets the brachial plexus. This approach is commonly performed for a variety of surgical procedures involving the shoulder, arm, and hand. Some examples include:
- Shoulder arthroscopy
- Rotator cuff repair
- ORIF of the arm or hand
- Distal biceps tendon repair
- Thumb arthroplasty
Overview of the Supraclavicular Block
The supraclavicular block involves depositing local anesthetic around the brachial plexus at the level of the distal trunks or origin of the divisions. At this location, all of the major branches of the brachial plexus are in close proximity and can be reliably blocked. As a result, you can use the supraclavicular block for most surgeries involving the upper extremity. You can use supraclavicular blocks as the primary anesthetic or in conjunction with general anesthesia to minimize pain and narcotic consumption, reduce opioid-related side effects, and shorten the length of stay in recovery.
Risks and Side Effects
Like other regional anesthesia techniques, supraclavicular blocks have risks related to the location where the block is performed. You can mitigate these risks through the use of ultrasound guidance. Some potential risks and side effects include:
- Phrenic nerve blockade
- Recurrent laryngeal nerve blockade
- Pneumothorax
- Local anesthetic systemic toxicity (LAST)
- Hematoma
- Infection
- Allergic reaction
- Horner syndrome
- Nerve injury
How to Perform a Supraclavicular Block
After passing between the anterior and middle scalene muscles, the nerve roots of the brachial plexus divide into 3 trunks: superior, middle, and inferior. These structures will then travel down the neck toward the clavicle to form the 6 divisions. Within the supraclavicular region, the brachial plexus lies adjacent to the subclavian artery, first rib, and pleura.
To perform the block, place the ultrasound transducer in a transverse position over the lower neck, superior to the clavicle. The pulsating subclavian artery and brachial plexus can be easily identified. Insert the block needle through the skin 1-2cm lateral to the transducer and advanced in-plane until the needle tip is adjacent to the brachial plexus. Administer 3-5ml incremental doses of local anesthetic up to a total volume of 15-20ml. Reposition the needle around the brachial plexus to help facilitate local anesthetic spread. To ensure reliable blockade of the ulnar nerve, local anesthetic should be deposited within the corner pocket, which is formed by the borders of the brachial plexus, subclavian artery, and first rib. For a more comprehensive and detailed review of this block, use the Block Buddy Pro app.
Get Complete Instructions in the Block Buddy Pro App
Block Buddy Pro is the latest resource to help anesthesia providers administer ultrasound-guided nerve blocks. Particularly, the app includes a Supraclavicular Block Lesson that includes:
- A detailed list of equipment.
- Detailed illustrations and ultrasound images to guide you further.
- A narrated video with step-by-step instructions.
- Clinical pearls, an Rx guide, and more!
You will also gain access to other comprehensive lessons regarding a variety of blocks, and in-depth reviews of the nerve plexus, and point-of-care ultrasound. You can also add essential notes directly in the app, and have access to them online or offline. Block Buddy Pro is available on all devices (mobile, tablet, and desktop) and can be purchased in the App Store and Google Play Store. Create your account now!
